Table of Contents
Aspects of efficient ventilation in hospitals
Identifying energy-conservation potential
The baseline study on implementing the Passive House concept in hospitals studied energy-conservation potential in the planning stage [Kah et al 2013]. This paper presents the insights gained in the baseline study regarding energy-conservation potential in ventilation systems used in hospitals within the context of hygiene requirements.
Certain areas of hospitals require great air flows, with especially high air exchange rates found in operation rooms, labs, and areas where utensils are sterilized. Ventilation systems therefore make up a significant share of total energy demand. In addition, a large number of individual components are needed to filter and purify the air in compliance with hygienic and functional requirements for individual hospital areas (especially operating rooms). The sum of these individual pressure losses has a great impact on ventilators' power consumption.
The main way that ventilation systems can be tweaked to improve operational efficiency is by optimizing the design and outdoor air demand controls along with reducing pressure losses for individual components. The baseline study also looked into the extent to which heat recovery systems can be used in hospital ventilation systems. Requirements for areas covered under DIN1946-4 were taken into account in the investigation of energy-conservation potential.
Demand and control of outdoor air
Many areas in a clinic use medical devices with high cooling loads during operation and standby. The cooling load in specific rooms determines the need for outdoor air in a lot of ventilation plans for hospitals. By reducing cooling loads and decoupling cooling demand from the need for outdoor air, outdoor air exchange rates can be reduced considerably.
- Air exchange rates required for cooling demand should be determined based on the actual output data of medical devices with consideration of their time of use (simultaneity). Energy-efficient devices reduce not only power demand for medical technology, but also cooling demand – and hence the required air volume flows.
- Component cooling, distributed circulation units with cooling functions, etc. should be used so that ventilation units do not have to be excessively large in order to handle indoor heat loads.
Not all areas of a hospital are used around the clock. A lot of areas – labs, operating rooms, examination and treatment rooms, etc. – are only used on weekdays, and then only for around ten hours a day. There is great conservation potential in adapting ventilation to actual demand at specific times. A simple control system using flaps is good for rooms mainly used during normal business hours.
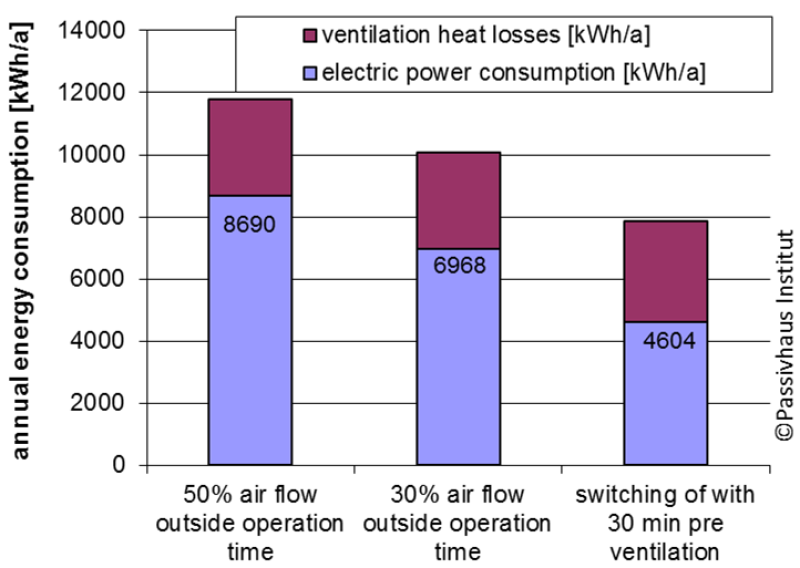
Need-based ventilation that switches off outside of business hours is even possible in operating rooms (in accordance with ÖNORM 6020). Room-specific patient-oriented features are generally only needed when the operating room is in use. To ensure proper hygiene in the operating room, ventilation should be ramped up to the design volume flow 30 minutes before the room is used. In this way, the energy required to run ventilators can be reduced by around 65 percent compared to the level required for around-the-clock operation. Up to now, hospitals have generally not tapped this potential. A study conducted by the Fraunhofer Institute on energy consumption in hospitals looked into reducing the volume flow of ventilation systems for operating rooms outside of normal hours [Beier 2009]. It was found that the operating volume flow was only reduced to 55 percent on average outside of normal hours in the operating rooms investigated.
When ventilation systems are turned off when operating rooms are not used and switched on again 30 minutes beforehand, their annual power consumption can be reduced by around 45 percent more than if volume flow is only reduced 50 percent outside of operating hours. In light of the enormous amounts of air required in DIN 1946-4 for most operating rooms (1,200 m³/h of outdoor air + ca. 8,000 m³/h of circulated air), the feasible energy savings are considerable (see Figure 1). On the other hand, more moderate approaches for air flows tailored to the number of people present should be pursued in areas not covered by DIN 1946 in cooperation with the building owner. In examination rooms, 30 m³/h per person is recommended, in line with recommendations for residential buildings.
Preventing high pressure losses in the duct network
The baseline study on implementing the Passive House concept in hospitals looked into ways of reducing pressure losses in individual components. Target values for ventilation units' power consumption were derived from the feasible individual pressure losses. If components are properly dimensioned, the target value can be 0.45 Wh/m³ even in hospitals. Air filtration often accounts for a lot of the overall pressure loss in a ventilation system. The greater hygiene requirements in hospitals make the situation even more difficult because the filters required often have two or three stages.
[DIN EN 13779] specifies recommendations for maximum final pressure losses from filters ranging from 100 Pa to 250 Pa for M7 filters. To reduce energy demand for filtration, final pressure losses have to be lowered considerably. Filters need to be replaced at least once a year, and the initial pressure loss needs to be reduced in order to additionally limit final pressure losses. If the filters are properly dimensioned, initial pressure losses for M7 filters can remain at 50 Pa, as the ventilation devices certified as Passive House components with outputs greater than 600 m³/h show. Some devices even have much lower initial pressure losses.
The F9 filters commonly recommended in hospitals for the second filter stage can also be dimensioned to lower pressure losses. [Kah et al 2013] recommends an initial pressure loss of 70 Pa for F9 filters. The final filter stage, H13, causes the greatest pressure losses in hospitals along with heat recovery. The enormous amounts of air that need to flow through a terminal H13 filter in a functional area make it clear that a properly dimensioned filter here will have a much greater effect on lowering pressure losses – and, thus, energy consumption – than at the first and second filter stages. Airborne-particle filters are generally designed for an initial pressure loss of 250 Pa according to manufacturers. For the filtering of airborne particles at the final stage (HEPA filters), [DIN EN 13779] even specifies pressure losses of 400 to 700 Pa. The filter area of such filters can also be made larger to reduce pressure losses considerably. There are two ways to enlarge the filter area:
- Make the filter outlet area larger, or
- make the filter deeper.
Filters at the final stage (where the filter element is directly integrated in the air outlet) can easily have larger outlet areas than filters integrated in central units.
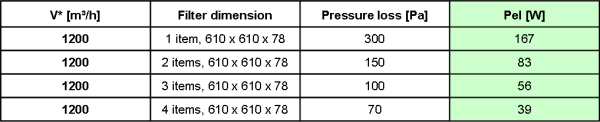
The following table shows the influence of the filter outlet area on pressure losses, and hence on energy demand stemming from the filter.
If the filter outlet surface is tripled (from one to three elements), pressure losses can be reduced by a third. Power demand also drops by a third. Pressure losses can even be reduced to 70 Pa if four outlet elements are used. To limit the expansion of the filter outlet surface, the filter depth can also be increased in order to reduce pressure losses.
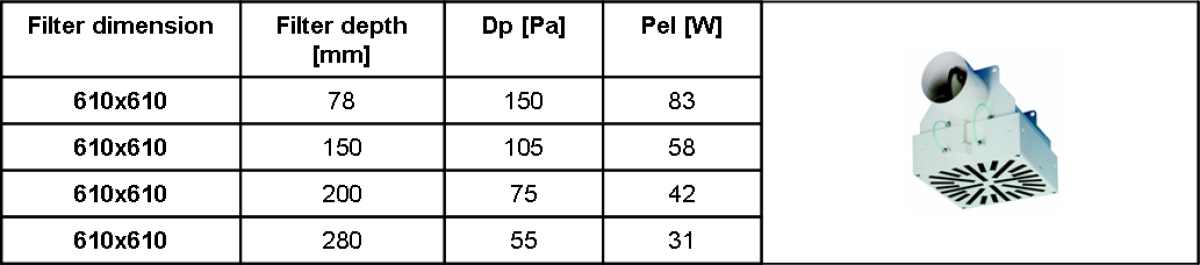
The following table compares the impact of different filter depths on pressure loss with the same filter outlet area and fresh air volume flow.
Doubling the filter depth from 78 mm to 150 mm can reduce pressure losses by a third. Pressure losses < 75 Pa are even possible for airborne-particle filters with a depth of > 200 mm.
Unfortunately, it is harder to use deeper filters in the final filtration stage than it is to enlarge the filter outlet area. Standard outlet elements usually have a frame for a filter depth of 78 mm. Deeper outlet elements can thus increase investment costs. Hopefully, demand for such “special solutions” to reduce operating costs will become more common, so that supply will go up – and prices down.
Adjusting filters is certainly the main way to reduce pressure losses in hospitals. The following benchmarks apply for initial filter pressure losses for efficient ventilation systems:
| M7 ≤ 50 Pa | F9 ≤ 70 Pa | H13 ≤ 100 Pa |
When planning focuses on optimizing pressure losses, make sure the duct network is as compact as possible, especially where large amounts of air flow. When ventilation units are installed close to areas of consumption, low pressure losses make power consumption more efficient. Here, a compromise needs to be found between the close proximity of functional areas and equipment cabinets, on the one hand, and the shortest possible ducts for outdoor air and exhaust air, on the other.
Heat recovery in hospitals
The baseline study on implementing the Passive House concept in hospitals also looked into the extent to which heat recovery systems can be used in hospitals. It was found that hospital ventilation systems can have high-quality heat recovery (efficiency ≥ 75%). The study also took account of the special requirements for heat recovery in hygienically sensitive areas specified in DIN 1946-4.
Summary
The baseline study on implementing the Passive House concept in hospitals shows that a reduction in pressure losses in individual components, along with proper dimensioning and control of demand for outdoor air commensurate with actual demand, considerably reduces the energy consumption of hospital ventilation systems. If components are properly dimensioned, the target value can be 0.45 Wh/m³ even in hospitals.
References
[Kah et al 2013] O. Kah, K. Bräunlich, T. Schulz, A. Grill, O. Ottinger, R. Schumacher, Grundlagenstudie zur Umsetzung des Passivhauskonzept in Krankenhäusern / Baseline study on implementing the Passive House concept in hospitals, Studie im Auftrag des Hessischen Ministeriums für Wirtschaft, Verkehr und Landesentwicklung, Passivhaus Institut, Darmstadt 2013. (only available in German language)
[Beier 2009] Abschlussbericht Analyse des Energieverbrauchs und exemplarische Best-practice-Lösungen für relevante Verbrauchssektoren in Krankenhäusern; Dipl.-Ing. Carsten Beier, Fraunhofer-Institut für Umwelt-, Sicherheits- und Energietechnik UMSICHT, Oberhausen 2009
[DIN 1946-4] DIN 1946 Teil 4, Ausgabe: Dezember 2008: Raumlufttechnik - Teil 4: Raumlufttechnische Anlagen in Gebäuden und Räumen des Gesundheitswesens, DIN Deutsches Institut für Normung e.V., Beuth-Verlag, Berlin
[DIN EN 13779] DIN EN 13779, Ausgabe: September 2007: Lüftung von Nichtwohngebäuden-Allgemeine Grundlagen und Anforderungen für Lüftungs- und Klimaanlagen und Raumkühlsysteme, DIN Deutsches Institut für Normung e.V., Beuth-Verlag, Berlin
[ÖNORM 6020] ÖNORM H 6020, Ausgabe Februar 2007: Lüftungstechnische Anlagen für medizinisch genutzte Räume – Projektierung, Errichtung, Betrieb, Instandhaltung, technische und hygienische Kontrollen; Austrian Standards plus GmbH, Wien
See also
Overview of all articles on Passipedia about non-residential Passive House buildings
Overview of all articles on Passipedia about hospitals
Conference proceedings 18th International Passive House Conference 2014
List of all released conference proceedings of the 18th International Passive House Conference 2014 in Aachen